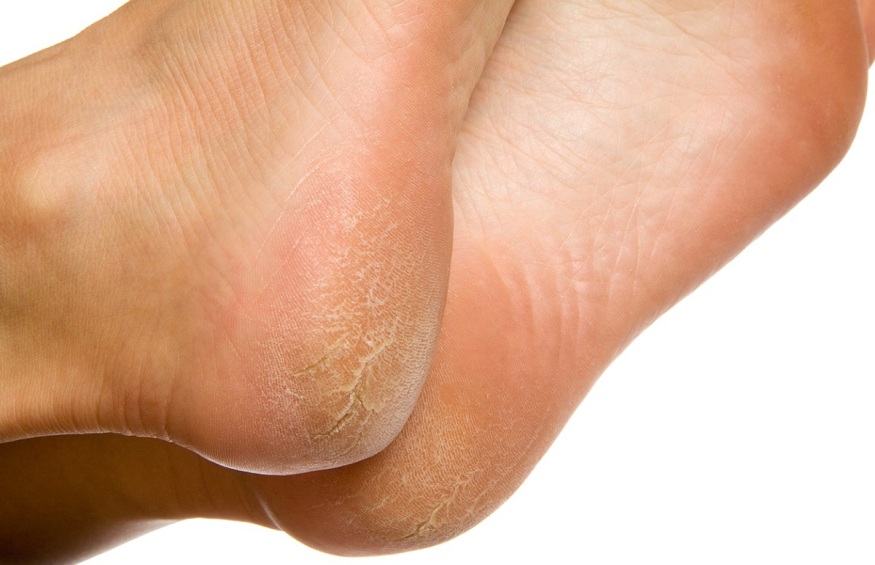
A cracked heel is a frequent foot condition. In most situations, the state is only an eyesore. Nevertheless, standing, walking, or applying pressure to the heel can be uncomfortable when the cracks or fissures get deep.
Causes
A cracked heel may happen to anyone. Predisposition might be caused by:
- Extremely dry skin
- Dermatitis atopy
- Plantar dermatosis in children
- Psoriasis
- Keratoderma palmoplantar
- Diabetes and hypothyroidism
Cracking begins with dry, thickened skin (corn and callus) around the rim of the heel. Then, increased pressure on the fat pad under the heel leads it to expand sideways, resulting in callus splitting or cracking. Some of the variables that lead to cracking or splitting are as follows:
- Obesity or being overweight
- Long periods of standing, especially on hard surfaces
- Shoes with open backs and sandals (no support for the fat pad under the foot)
Symptoms
The formation of dry, hard, thicker skin around the rim of the heel is the first indication of a cracked heel. A callus is a discoloured spot of skin that might be yellow or dark brown. Minor fractures appear over the callus at first. If left untreated, these fissures will get deeper as more pressure is applied to the heel, making walking and standing unpleasant. The fissures may get so deep that they bleed.
Cracked heels can develop infected and cause cellulitis in extreme situations. This requires elevation of the affected region, debridement of dead tissue, and antibiotics.
Cracked heels are especially concerning for diabetic patients, who may experience neuropathic damage (loss of feeling, notably in the feet) due to the fissures, which can develop into diabetic foot ulcers.
Treatment
The best way to cure cracked heels is total prevention. Simply massaging the heels with a moisturising lotion regularly can maintain the skin supple and moisturised. There are heel balms with descaling (keratolytic) or water-retaining (humectant) ingredients, such as:
- Salicylic acid
- Urea
- Saccharide isomerate
- Alpha-hydroxy acids
Feet should be examined regularly, and if cracking occurs, a moisturising regimen 2-3 times per day may be all that is required to repair the heel. Before applying moisturiser, gently scrape a pumice stone across the callus to remove some of the thick hard skin.
To alleviate discomfort, protect against infection, and promote faster healing, the fissures can be treated with a liquid, gel, or spray bandage.
A visit to a podiatrist may be necessary if the heels are badly damaged or if no progress is apparent after a week of self-treatment. Treatment options include the following:
- Debridement—the removal of tough, thick skin (this should not be attempted at home).
- Strapping is a bandage or dressing wrapped around the heel to limit skin mobility.
- Stronger softening or debriding treatments which are prescribed.
- Insoles, heel pads, or heel cups can help to disperse the weight of the heel and give more support (prevent the fat pad from expanding sideways)
Special tissue glue to keep the broken skin’s margins together so that it may mend.